Testosterone is the primary male sex hormone that plays a crucial role in men’s overall health and well-being. This hormone is responsible for regulating sex drive, sperm production, bone health, muscle mass, and energy levels throughout a man’s life.
Understanding normal testosterone levels in men is essential for maintaining optimal health and recognizing when medical intervention may be necessary. Testosterone deficiency can significantly impact quality of life, while maintaining healthy testosterone levels supports physical strength, mental clarity, and sexual function.
Key Takeaways
- Normal testosterone levels in men range from 265-923 ng/dL, with optimal levels between 450-600 ng/dL.
- Testosterone levels naturally decline by approximately 1% per year after age 30 as a normal part of aging.
- Low testosterone symptoms include reduced sex drive, fatigue, decreased muscle mass, and erectile dysfunction.
- Blood tests measuring total testosterone and free testosterone help determine if levels fall within the healthy range.
- Both natural methods and testosterone replacement therapy can address declining testosterone levels.
How is Testosterone Produced and Regulated?
The production of testosterone involves a complex feedback system that begins when the hypothalamus releases gonadotropin-releasing hormone (GnRH). This hormone signals the pituitary gland to release luteinizing hormone (LH) and follicle-stimulating hormone (FSH).
LH directly stimulates the testes to produce testosterone, while FSH supports sperm production and overall testicular function. The body maintains hormone balance through a feedback loop mechanism that adjusts production based on current testosterone levels and other hormones in the system.
Sex hormone-binding globulin (SHBG) plays a critical role in testosterone regulation by binding to the hormone and controlling how much free testosterone is available for the body to use. This binding process helps maintain stable serum testosterone concentrations and ensures proper hormone function throughout the body (National Library of Medicine).
What are the Normal Testosterone Levels by Age?
Testosterone levels naturally fluctuate throughout different life stages, with significant variations occurring from adolescence through older age. Understanding these age-related changes helps men and healthcare professionals determine whether testosterone levels fall within normal ranges for their specific age group.
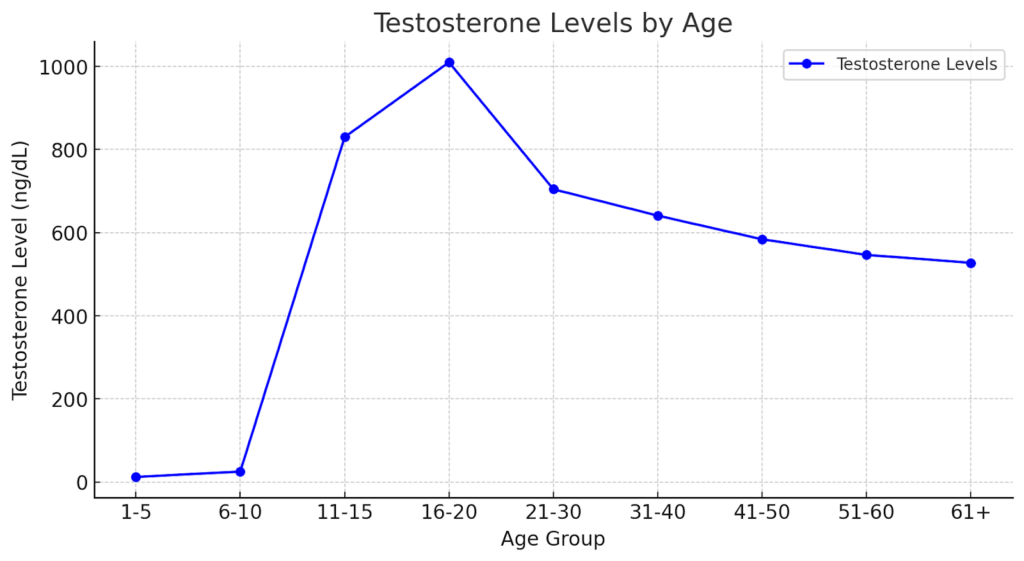
Normal Testosterone Ranges
The standard normal testosterone levels in men range from 265-923 nanograms per deciliter (ng/dL) in adult males. Most healthcare professionals consider levels between 450-600 ng/dL as optimal for maintaining good health and preventing symptoms of testosterone deficiency (Cleveland Clinic).
Normal ranges can vary depending on laboratory reference standards and testing methods used. The American Urological Association defines low testosterone as levels below 300 ng/dL, which typically requires medical evaluation and potential treatment.
Testosterone Levels in Adolescence and Early Adulthood
Peak testosterone levels occur during puberty and early adulthood when the hormone drives the completion of physical development. Testosterone levels are typically highest in the late teens and early twenties, often reaching the upper end of the normal range.
During this period, testosterone supports the development of adult male characteristics and establishes the foundation for lifelong hormone production. These elevated levels are essential for proper sexual development, bone density formation, and muscle mass establishment (Journal of Adolescent Health).
Testosterone Levels in Middle Age
A gradual decline in testosterone production typically begins around age 30, representing a normal part of the aging process. This decline occurs at approximately 1% per year, though the rate can vary depending on individual factors such as overall health, body fat percentage, and lifestyle choices (Cleveland Clinic).
This natural age-related decline affects various aspects of health, including energy levels, muscle mass maintenance, and sexual function. While some decline is normal, significant drops may indicate the need for medical evaluation and potential intervention.
Testosterone Levels in Older Men
Men over 60 often experience more pronounced decreases in testosterone levels, with many falling into the lower end of normal ranges. This age-related decline can lead to symptoms that significantly impact quality of life and overall well-being (National Library of Medicine).
The implications of low testosterone levels in older men extend beyond sexual health to include increased risk of osteoporosis, muscle weakness, and metabolic changes. Regular monitoring through blood tests helps healthcare professionals determine if testosterone therapy might be beneficial.
Are you Ready to take control of your hormone health?
Feel stronger, recover faster, and restore youthful energy—naturally. Let’s get started.What are the Symptoms of Abnormal Testosterone Levels?
Recognizing the signs and symptoms of abnormal testosterone levels helps men identify when they should seek medical evaluation. Both low and high testosterone levels can cause significant health issues that require professional attention.
Symptoms of Low Testosterone
Low testosterone levels produce several characteristic symptoms that can significantly impact daily life and overall health (Cleveland Clinic). The most common symptoms include:
- Reduced sex drive and erectile dysfunction
- Decreased muscle mass and increased body fat
- Persistent fatigue and low energy levels
- Bone density loss and increased fracture risk
- Weight gain, particularly around the midsection
- Depression and mood changes
- Difficulty concentrating and memory problems
- Irritability and increased stress sensitivity
- Reduced motivation and confidence
Symptoms of High Testosterone
While less common, elevated testosterone levels or hyperandrogenism can also cause health problems and uncomfortable symptoms. High testosterone levels may result from anabolic steroid use or certain medical conditions (Cleveland Clinic). Many common symptoms include:
- Severe acne and oily skin
- Male pattern baldness and excessive body hair
- Increased aggression and mood swings
- Sleep disturbances and restlessness
- Cardiovascular risks and blood pressure changes
How to Manage Abnormal Testosterone
Managing abnormal testosterone levels requires a holistic approach that includes medical treatment, lifestyle modifications, and ongoing monitoring. Healthcare professionals, like those at Huddle Men’s Health, determine the most appropriate treatment strategy based on individual symptoms, testosterone test results, and overall health status.
Testosterone Replacement Therapy (TRT)
Testosterone replacement therapy offers several treatment options for men with clinically low testosterone levels. Each method has unique benefits and considerations:
TRT Options:
- Testosterone injections: Administered weekly or bi-weekly by medical professionals or at-home self-administered injections for consistent hormone levels.
- Transdermal patches: Applied daily for steady hormone absorption.
- Topical gels: Easy application with good absorption rates, but there is a risk of contacting others.
- Testosterone pellets: Implanted every 3-6 months for long-term hormone delivery, but leave a medical device under the skin.
Benefits of TRT include:
- Improved sex drive and erectile function
- Increased muscle mass and bone density
- Enhanced energy levels and mood
- Better cognitive function and concentration
TRT works by supplementing the body’s natural testosterone production to restore normal hormone levels. Medical supervision and regular monitoring are essential to ensure safety and effectiveness while minimizing potential risks and side effects.
Natural Ways to Support Testosterone Levels
Many men can support healthy testosterone levels through lifestyle modifications and natural approaches. These methods work best for men with mild deficiencies or those looking to optimize their hormone health:
Exercise and Physical Activity:
- Resistance training and weightlifting
- High-intensity interval training (HIIT)
- Regular cardiovascular exercise
- Avoiding excessive endurance training
Dietary Approaches:
- Maintain adequate protein intake
- Include healthy fats in your diet
- Limit processed foods and excess sugar
- Maintain proper caloric balance
Lifestyle Modifications:
- Prioritize 7-9 hours of quality sleep
- Manage stress through relaxation techniques
- Maintain a healthy body weight
- Limit alcohol consumption
- Avoid smoking and recreational drugs
Supplements and Nutrition for Testosterone
Certain vitamins and minerals play important roles in testosterone production and hormone regulation. Evidence-based supplements may provide additional support when combined with healthy lifestyle practices:
Key Nutrients for Testosterone Support:
- Vitamin D: Essential for hormone production and regulation
- Zinc: Critical for testosterone synthesis and male reproductive health
- Magnesium: Supports hormone balance and muscle function
- Vitamin B6: Helps regulate hormone metabolism
Realistic expectations are essential when considering supplements, as they typically provide modest benefits compared to medical treatment. Supplements work best as part of a comprehensive approach that includes proper nutrition, exercise, and stress management.
Support Healthy Testosterone Levels with Huddle Men’s Health
Understanding normal testosterone levels in men empowers you to make informed decisions about your health and well-being. Regular monitoring, healthy lifestyle choices, and professional medical guidance when needed can help maintain optimal hormone levels throughout your life.
Whether you’re experiencing symptoms of low testosterone or simply want to optimize your hormone health, it’s never too late to take proactive steps. The combination of natural remedies and medical treatment, when appropriate, offers the best outcomes for long-term health and vitality.
Take the first step toward optimal hormone health with Huddle Men’s Health. Contact us today to schedule your testosterone assessment and discover how we can help you achieve your health goals.
Normal Testosterone Level FAQs
What are considered normal testosterone levels for men?
Normal testosterone levels for men range from 265-923 ng/dL, with optimal levels between 450-600 ng/dL. The American Urological Association defines low testosterone as levels below 300 ng/dL. Individual symptoms matter more than exact numbers when determining if treatment is needed.
How do testosterone levels change with age?
Testosterone levels naturally decline by about 1% per year starting around age 30. This gradual decrease is a regular part of aging and affects energy, muscle mass, and sexual function. Significant drops or troublesome symptoms may require medical evaluation.
What should I do if my testosterone levels are low?
Consult a healthcare professional who specializes in hormone health for proper evaluation and treatment recommendations. Treatment options include testosterone replacement therapy, lifestyle changes, or addressing underlying health conditions. Never attempt to self-treat low testosterone without medical supervision.
How can I naturally boost my testosterone levels?
Focus on strength training, maintaining a healthy weight, getting 7-9 hours of sleep, and managing stress effectively. Eat adequate protein and healthy fats while limiting processed foods and excess alcohol. Natural methods work best for mild deficiencies but may not be sufficient for clinically low levels.
Is testosterone replacement therapy safe?
Testosterone replacement therapy is generally safe when properly supervised by qualified healthcare professionals. Benefits typically outweigh risks for men with clinically diagnosed low testosterone and related symptoms. Regular monitoring helps minimize potential side effects and ensures optimal treatment outcomes.
How often should I get my testosterone levels tested?
Men over 40 with low testosterone symptoms should consider annual testing as part of routine health screenings. During testosterone therapy, testing occurs more frequently initially, then every 3-6 months once levels stabilize. Your healthcare provider will determine the appropriate testing schedule based on your individual needs.

